Many people think diabetes begins with obvious symptoms like extreme thirst or constant fatigue. While those signs are common, the body often sends quieter warnings much earlier — especially through the feet.
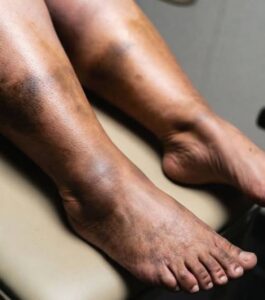
Your feet can reveal changes in circulation, nerve health, and healing ability long before diabetes is officially diagnosed. That is why doctors frequently examine the feet during routine diabetes checkups. High blood sugar affects blood vessels and nerves over time, and because the feet sit farthest from the heart, they are often the first area where problems appear.
Ignoring these warning signs can lead to serious complications later. However, recognizing them early may help people seek medical care sooner and prevent long-term damage.
Many adults dismiss unusual foot symptoms as simple aging, standing too long, or wearing uncomfortable shoes. Yet persistent tingling, numbness, or slow-healing wounds may point to something deeper happening inside the body.
A middle-aged man once noticed that his feet constantly felt “asleep” at night. He assumed poor posture or tight shoes were causing the problem. Months later, he developed a small blister that took weeks to heal. After finally visiting his doctor, routine testing revealed Type 2 Diabetes. Fortunately, early treatment helped him control his blood sugar before more severe complications developed. His experience highlights how easy it is to overlook subtle symptoms until they become impossible to ignore.
Why Diabetes Often Affects the Feet First
High Blood Sugar Damages Nerves
One of the most common complications of diabetes is peripheral neuropathy, a condition caused by nerve damage.
When blood sugar levels remain elevated for long periods, tiny blood vessels that nourish the nerves begin to weaken. Over time, the nerves struggle to function properly.
This damage often starts in the feet because the nerves there are especially long and vulnerable.
Symptoms may include:
- Tingling
- Burning
- Numbness
- Sharp pain
- Reduced sensation
Some people notice symptoms mainly at night, while others experience discomfort throughout the day.
Unfortunately, nerve damage may progress slowly and silently. Many individuals do not realize they have diabetes until neuropathy has already begun.
Circulation Problems Develop Gradually
Diabetes also affects circulation by damaging blood vessels.
Healthy blood flow is essential because it delivers oxygen and nutrients throughout the body. When circulation becomes impaired, the feet may suffer first due to their distance from the heart.
Poor circulation can lead to:
- Cold feet
- Swelling
- Skin discoloration
- Slow wound healing
- Leg cramps during walking
Reduced blood flow also increases infection risk because the body struggles to repair damaged tissue efficiently.
This combination of nerve damage and poor circulation makes diabetic foot complications especially dangerous if ignored.
Tingling, Burning, and Numbness
Persistent Tingling Sensations
One of the earliest warning signs of diabetic neuropathy is persistent tingling or “pins and needles.”
Many people describe it as:
- A crawling sensation
- Electrical tingling
- Feet “falling asleep”
- Mild buzzing sensations
At first, symptoms may come and go. Over time, they often become more frequent.
Tingling occurs because damaged nerves send abnormal signals to the brain.
Although temporary tingling occasionally happens from sitting awkwardly or crossing legs, persistent symptoms deserve medical attention.
Burning Feet and Loss of Sensation
Some individuals experience burning sensations in the feet even when the skin feels cool to the touch.
Burning pain may worsen:
- At night
- After walking
- During rest
- In warm environments
Others experience the opposite problem: numbness.
Numbness may seem harmless initially, but it can become dangerous because people lose the ability to feel injuries.
Someone with severe neuropathy may:
- Step on sharp objects unknowingly
- Develop blisters without noticing
- Fail to feel cuts or infections
Loss of protective sensation significantly increases the risk of ulcers and complications.
Slow-Healing Wounds and Skin Changes
Cuts and Blisters That Heal Slowly
Healthy skin repairs itself quickly after minor injuries. Diabetes interferes with this process because high blood sugar weakens circulation and immune function.
Small injuries may become major problems if healing slows down.
Warning signs include:
- Cuts lasting weeks
- Persistent sores
- Cracked skin
- Blisters that worsen
- Redness around wounds
Even tiny injuries should not be ignored if healing seems unusually slow.
Diabetic foot ulcers are one of the most serious complications linked to uncontrolled diabetes. Early treatment greatly reduces risks.
Dry, Cracked, or Discolored Skin
Nerve damage may affect sweat and oil production in the feet, causing excessive dryness.
Cracked heels may develop as skin loses moisture and elasticity.
These cracks can become entry points for bacteria and infections.
People with diabetes may also notice:
- Shiny skin
- Hair loss on the legs
- Pale feet
- Purple or reddish discoloration
Changes in skin appearance often suggest circulation problems.
Monitoring the skin carefully helps identify issues before they worsen.
Swelling and Pain While Walking
Swollen Feet and Ankles
Swelling, also called edema, can happen for many reasons. However, diabetes-related circulation issues may contribute to persistent swelling in the lower legs and feet.
Signs include:
- Tight shoes
- Sock marks on the skin
- Puffy ankles
- Heaviness in the feet
Swelling may become worse after long periods of standing or sitting.
Diabetes may also affect kidney function, which can contribute to fluid retention.
Although swelling does not always mean diabetes is present, persistent edema combined with other symptoms should not be ignored.
Leg Pain During Walking
Some people with diabetes develop peripheral artery disease, a condition where narrowed blood vessels reduce blood flow to the legs.
This may cause pain called claudication.
Symptoms include:
- Cramping during walking
- Aching calves
- Foot fatigue
- Pain relieved by rest
Because the muscles receive less oxygen-rich blood, activity becomes uncomfortable.
Reduced circulation also increases the risk of ulcers and infections.
Repeated Infections and Foot Shape Changes
Fungal Infections Can Become Frequent
High blood sugar creates an environment where fungi and bacteria thrive more easily.
People with diabetes may develop repeated:
- Athlete’s foot
- Toenail fungus
- Skin infections
- Yeast infections
Toenails may become:
- Thickened
- Yellow
- Brittle
- Crumbly
Persistent fungal infections can signal underlying blood sugar issues, especially when combined with other symptoms.
Structural Changes in the Feet
Advanced nerve damage may weaken muscles in the feet over time.
This can gradually alter foot structure and shape.
Possible changes include:
- Hammertoes
- Fallen arches
- Toe deformities
- Changes in shoe fit
Some individuals notice their shoes suddenly feel tighter or less supportive.
Because sensation may already be reduced, structural changes sometimes progress unnoticed.
Routine foot exams help detect these issues early.
Why Early Detection Matters
Diabetes Complications Often Progress Slowly
One dangerous aspect of diabetes is that symptoms may develop gradually over years.
Many people adapt to subtle discomforts without realizing their health is changing.
Unfortunately, untreated diabetes increases the risk of:
- Severe neuropathy
- Foot ulcers
- Infections
- Kidney disease
- Vision loss
- Heart disease
Recognizing warning signs early can prevent many complications.
Simple blood tests can identify:
- Prediabetes
- Elevated blood sugar
- Type 2 Diabetes
Early treatment often includes lifestyle changes that dramatically improve long-term outcomes.
Small Changes Can Protect Foot Health
Protecting the feet becomes especially important for individuals with diabetes or prediabetes.
Helpful habits include:
- Checking feet daily
- Wearing supportive shoes
- Avoiding barefoot walking
- Moisturizing dry skin
- Keeping toenails trimmed carefully
- Monitoring cuts and blisters
Even small preventive actions can reduce complications significantly.
Managing Blood Sugar and Supporting Nerve Health
Lifestyle Habits Matter
Healthy lifestyle habits play a major role in blood sugar control and circulation.
Key habits include:
- Balanced nutrition
- Regular exercise
- Weight management
- Stress reduction
- Adequate sleep
Physical activity improves circulation and insulin sensitivity, helping the body manage glucose more effectively.
Nutrition also affects nerve health and inflammation throughout the body.
Medical Care Is Essential
Anyone experiencing persistent foot symptoms should speak with a healthcare professional.
Doctors may recommend:
- Blood sugar testing
- A1C testing
- Circulation exams
- Nerve evaluations
- Foot screenings
Managing diabetes early greatly lowers the risk of severe nerve and circulation damage.
Routine monitoring helps prevent small problems from becoming emergencies.
Common Myths About Diabetes and Foot Symptoms
Myth: Only Older Adults Develop Diabetes
Type 2 Diabetes is becoming increasingly common among younger adults and even teenagers.
Foot symptoms can occur at various ages.
Myth: Foot Numbness Is Normal Aging
Occasional discomfort may happen with age, but persistent numbness or tingling should always be evaluated.
Myth: Diabetes Symptoms Always Appear Suddenly
Many symptoms develop gradually over years.
Early signs are often subtle and easy to overlook.
Myth: Only Severe Diabetes Causes Foot Problems
Even prediabetes may contribute to nerve and circulation changes in some individuals.
Myth: Foot Problems Are Harmless
Ignoring diabetic foot symptoms may lead to ulcers, infections, and serious complications if untreated.
Frequently Asked Questions
Can tingling feet mean diabetes?
Yes. Persistent tingling may be an early sign of diabetic neuropathy caused by nerve damage from high blood sugar.
Are swollen feet always related to diabetes?
No. Swelling has many possible causes, but diabetes-related circulation or kidney issues may contribute.
Can diabetic nerve damage improve?
Early nerve damage may improve when blood sugar levels are controlled consistently.
Why do wounds heal slowly with diabetes?
High blood sugar weakens circulation and immune function, making tissue repair slower.
Should I see a doctor for numb feet?
Yes. Persistent numbness, tingling, or burning sensations should be medically evaluated.
Conclusion
Your feet can reveal valuable clues about your overall health long before serious complications develop. Tingling, numbness, burning sensations, swelling, slow-healing wounds, and circulation changes may all point toward underlying blood sugar problems.
Although these symptoms do not automatically mean diabetes is present, they should never be ignored when persistent or worsening.
Early detection matters because diabetes-related nerve and circulation damage often progresses gradually over time. Recognizing warning signs early allows people to seek treatment, improve blood sugar control, and protect long-term health.
Healthy habits, regular medical care, and daily foot awareness can make a major difference in preventing complications.
Sometimes the body whispers before it screams. Paying attention to your feet may help you catch important health issues before they become far more serious.